Abstract
Osteochondromas are the commonest bone tumors. They cease to grow post skeletal maturity and are rarely malignant(1%), thus making the indications for their excision very minimal. Diagnosis is usually confirmed on a radiograph, since most are asymptomatic, a conservative protocol is followed. Rapid increase in size, especially after skeletal maturity, pain, a cartilage cap of more than 2cm are all indications of a malignant lesion and need definitive diagnosis and surgery. Our case, presented with a lesion in an unusual location for osteochondroma, which was large enough to be symptomatic, thus leading to our management being aggressive, including excision, biopsy with a definitive diagnosis and plate fixation. Thus emphasizing the need to suspect osteochondromas in unusual locations and surge for definitive diagnosis in aggressive lesions.
Introduction
Osteochondroma is a benign osteo-cartilaginous tumor of originating from metaphysis of long bones, usual sites being the knee, ankle, shoulder and forearm These are usually asymptomatic and incidental findings. They are also mostly extra-articular and grow away from epiphysis1.They can rarely be symptomatic, when they compress surrounding structures( tendon, joint capsule, bursa), malignant transformation, pathological fracture of stalk or compression of neurovascular structures2,3,4 Intra-articular osteochondromas can be symptomatic earlier that extra-articular in the form of painful range of motion or joint stiffness or leg- length discrepancy. Osteochondroma of or around the hip joint, causing block in range of motion and pain is a not so rare a condition now in children. Management options in such children are many ranging from conservative, surgical excision and plate fixation. We present a case of a large, pedunculated lesion arising from proximal femoral metaphysis, which created a diagnostic dilemma since it could be heterotopic ossification, chondrosarcoma, synovial chondromatosis or an osteochondroma. We managed this with surgical excision and fixation with LCP as prophylaxis for fracture with good results and histopathology of the lesion to get to a sure diagnosis.
Case Report(s)
A 10-year-old male child presented to our outpatient department with complaints of difficulty in squatting for 2 year and right hip pain for 6 months
The patient had visited multiple doctors previously and was given pain relief medications, which would only provide temporary pain relief. The patient was referred to our center by the doctor, due to the appearance of a large bony lesion on x-ray which he suspected to be malignant. There was no history of any trauma or snapping sound from the hip while playing. The patient noticed difficulty in squatting from 2 years due to a mehanical block of flexion which was progressive. From 6 months Patient also complain of pain in Right Hip which occurred on walking and squatting. The pain was insidious in onset and gradually progressive, no history of night pain or rest pain. On examination, the patient had an antalgic gait, a bony, non-mobile swelling of size 10x8 x 4cm(AP, medial-lateral & proximal-distal respectively) on the anteromedial aspect of the thigh, and restricted flexion, adduction and Internal rotation which are painful in extreme of motion.
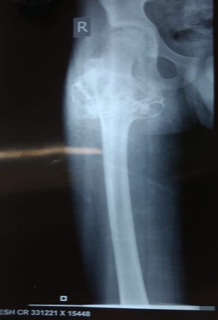
Orthogonal radiographs of the pelvis with bilateral hips and right hip with femur were ordered. Radiographs showed a cauliflower-like growth from anterior femoral cortex involving the greater trochanter, no cortical breach, no other lesions, no loose bodies in the joint, and no pathological fracture.
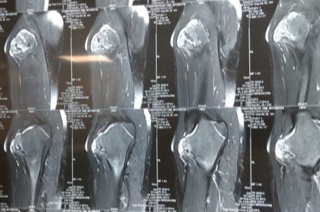
Considering this a large and symptomatic lesion we ordered for an MRI. MRI was suggestive of a lesion originating from proximal femoral metaphysis, with medullary canal continuous with the femur, with the involvement of greater trochanter and bone expansion but did not breach the cortex. This was suggestive of an osteochondroma in an unusual location.
We discussed the need for surgery since this was a large and symptomatic osteochondroma of an unusual location and even a minimal risk of transformation needed to be negated. We also realized that excision of lesion of this size, will weaken the bone and need a prophylactic fracture stabilization procedure. We kept options of a Dynamic Hip Screw(Pediatric), Angle Blade Plate, LCDCP and a Distal femoral locking plate, which we would use in a reverse fashion for stabilization.
The surgical decision, procedure, and outcomes were discussed at length with the patient and parents, who consented for surgery and biopsy to reach a confirmatory diagnosis.
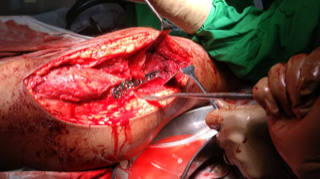
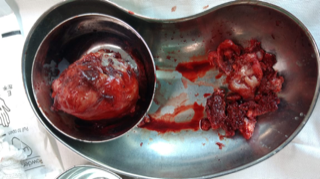
An anterolateral Watson Jones approach was used to expose the lateral and anterior aspect of the lesion. An extended approach was used to ensure extra-periosteal excision to avoid re-occurrences. Once excision was complete, a void was created which needed to be dealt with. As decided pre-operatively, we used a distal femoral locking plate, in a reverse order to adjust for the contour of the greater trochanter and fixed the bone. For bridging the void created by excision we filled the void with iliac crest bone graft.
POST-OPERATIVE
The patient was kept no weight bearing for 6 weeks, after which partial and then full weight bearing was gradually started over the next 4-6 weeks. The patient at 6 months, was pain-free, with a 120 degree flexion as compared to 130 degree of the normal side, 40 degree abduction as compared to 45 degree of normal side, 25 degree adduction as compared to 30 degree of normal side, 40 degree of internal and external rotation which was comparable to other side. The patient was able to sit cross-legged and squat.
Table 1 - Range of motion(in degrees) before and after surgery
|
|
Pre-operative ROM
|
Post-operative ROM
|
|
Flexion
|
90
|
120
|
|
Extension
|
5
|
10
|
|
Abduction
|
30
|
40
|
|
Adduction
|
5
|
25
|
|
External Rotation
|
30
|
40
|
|
Internal Rotation
|
20
|
40
|
1) preoperative radiographs and MRI
2) Intraoperative images and specimen
DISCUSSION
Osteochondroma is the most common benign tumor of bone, has both osteo-cartilaginous components, has a medullary canal continuous with that of parent bone, is usually extra-articular and grows away from the joint. Most common sites are the rapidly growing epiphysis, namely distal femur, proximal tibia, and proximal humerus.(5) Growth usually stops at skeletal maturity, and growth after this is considered to be a sign of malignant transformation.(5) The proximal femur is an uncommon site of osteochondroma. There are case reports which emphasize that proximal femoral, acetabular and intra-articular osteochondromas can cause pain, stiffness, snapping and even sciatic nerve compression, making them an important entity to be considered for surgical excision before they become symptomatic. Saglik et al had only 4.8% cases of proximal femur out of all the 313 cases described.6
Multiple Hereditary Exostosis (MHE) is a hereditary form of multiple exostosis or osteochondromas, although single lesions are found in about 85% of those diagnosed with osteochondroma.5 Hip involvement in MHE is common and presents with a different set of complications like coxa Valga, increased femoral ante-version or overgrowth of femoral neck.4 Rather in solitary osteochondroma of hip present with compressive complaints of bursitis, snapping2, sciatic nerve palsy7,3 or restriction of motion due to mechanical blockade or femoro-acetabular impingement7.
The risk of malignant transformation is indicated by raid increase in size, especially after skeletal maturity, new onset pain, pathological fracture or a cartilage cap thickness of >2cm. solitary lesions have a risk of 1-2%8 whereas MHE have a risk of 1-25%.9 Any doubts about malignant transformation need to be negated on histopathology after biopsy, as malignant transformation is one of the most severe complications of an osteochondroma.
Being a large, symptomatic, and presentation at an unusual location, all indicated towards an aggressive lesion, needing an excision biopsy, a confirmatory diagnosis, exclusion of malignant potential, improvement in symptoms and stabilization.
Biopsy, though rarely needed, can be a core needle, but is more often excisional, since it also relieves the patient of cosmetic complaints of swelling or any compressive symptoms if present. A complete extra-periosteal excision, with complete removal of cartilage cap is a must to avoid any re-occurrences which is approximated to be present in about 2% cases.10,11 Larger osteochondromas, especially in proximal femoral metaphysis, present with the problem of need of stabilization, being an area of high shear forces, and a void or weakening of bone in this area can lead to a very high risk of fracture. Multiple fixation devices in the form of threaded screws, blade plates, LCDCP and locking plates along with bone graft for voids, if any created are available. Blade plates and screws are good options if intra-articular or peritrochantric involvement are present, where as LCDCP’s and locking plates can be used for extra-articular fixation. We have had a good experience with using a distal femoral locking plate, in a reverse fashion to act like a proximal femoral locking plate. This provides a well contoured fit for the proximal femur and adequate fixation without disturbing the intra-articular anatomy.
CONCLUSION
Osteochondromas are very common lesions in skeletally immature, and can present in locations where the orthopaedician might not keep them as a first differential. Also these unusual sites of presentation need newer methods of management, biopsy and fixation. The surgeon should always approach such lesions with suspicion and manage them aggressively to provide symptomatic relief as well as negate any evidence of malignancy.
REFRENCES
1.Azar FM, Beaty JH, Canale ST. Campbell’s Operative Orthopaedics. 13th editi. Elsevier; 2017. 938-942 p.
2.Inoue S, Noguchi Y, Mae T, Rikimaru S, Hotokezaka S. An external snapping hip caused by osteochondroma of the proximal femur. Mod Rheumatol. 2005 Dec 20;15(6):432–4.
3.Turan Ilica A, Yasar E, Tuba Sanal H, Duran C, Guvenc I. Sciatic nerve compression due to femoral neck osteochondroma: MDCT and MR findings. Clin Rheumatol. 2008 Mar 17;27(3):403–4.
4.Am El-Fiky T, Chow W, Li YH, To M. Hereditary multiple exostoses of the hip. Vol. 17, Journal of Orthopaedic Surgery. 2009.
5.Czerniak B. Bone Tumors. 2nd editio. Elsevier; 2016.
6.Saglik Y, Altay M, Unal VS, Basarir K, Yildiz Y. Manifestations and management of osteochondromas: a retrospective analysis of 382 patients. Acta Orthop Belg. 2006 Dec;72(6):748–55.
7.Mondal S, Chowdhury A, Mandal PK, Roy D, Pal S, Gazi E, et al. Osteochondroma of femoral neck-a rare cause of femoro-acetabular impingement and sciatic nerve compression. Vol. 13, IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-ISSN. 2014.
8.Garrison RC, Unni KK, McLeod RA, Pritchard DJ, Dahlin DC. Chondrosarcoma arising in osteochondroma. Cancer. 1982 May 1;49(9):1890–7.
9.Peterson HA. Multiple hereditary osteochondromata. Clin Orthop Relat Res. 1989 Feb;(239):222–30.
10.Humbert ET, Mehlman C, Crawford AH. Two cases of osteochondroma recurrence after surgical resection. Am J Orthop (Belle Mead NJ). 2001 Jan;30(1):62–4.
11.Bottner F, Rodl R, Kordish I, Winklemann W, Gosheger G, Lindner N. Surgical treatment of symptomatic osteochondroma. A three- to eight-year follow-up study. J Bone Joint Surg Br. 2003 Nov;85(8):1161–5.
author contributions
Dr.Prashant Kumar Sharma
Acquisition of data, assistant in surgery and planning
Dr.Pulak Vatsya
Drafting of article, Critical revision of article, Assistant in surgery and planning
Dr.Pebum Sudesh
Primary surgeon, Concept and design
Dr.G.Nirmal Raj
Acquisition of data, Revision of article
Dr.Karthick Rangaswamy
Assistant in surgery and planning, Concept and design
illustrations
Illustration 1: Clinical picture of child showing rocker- bottom foot.
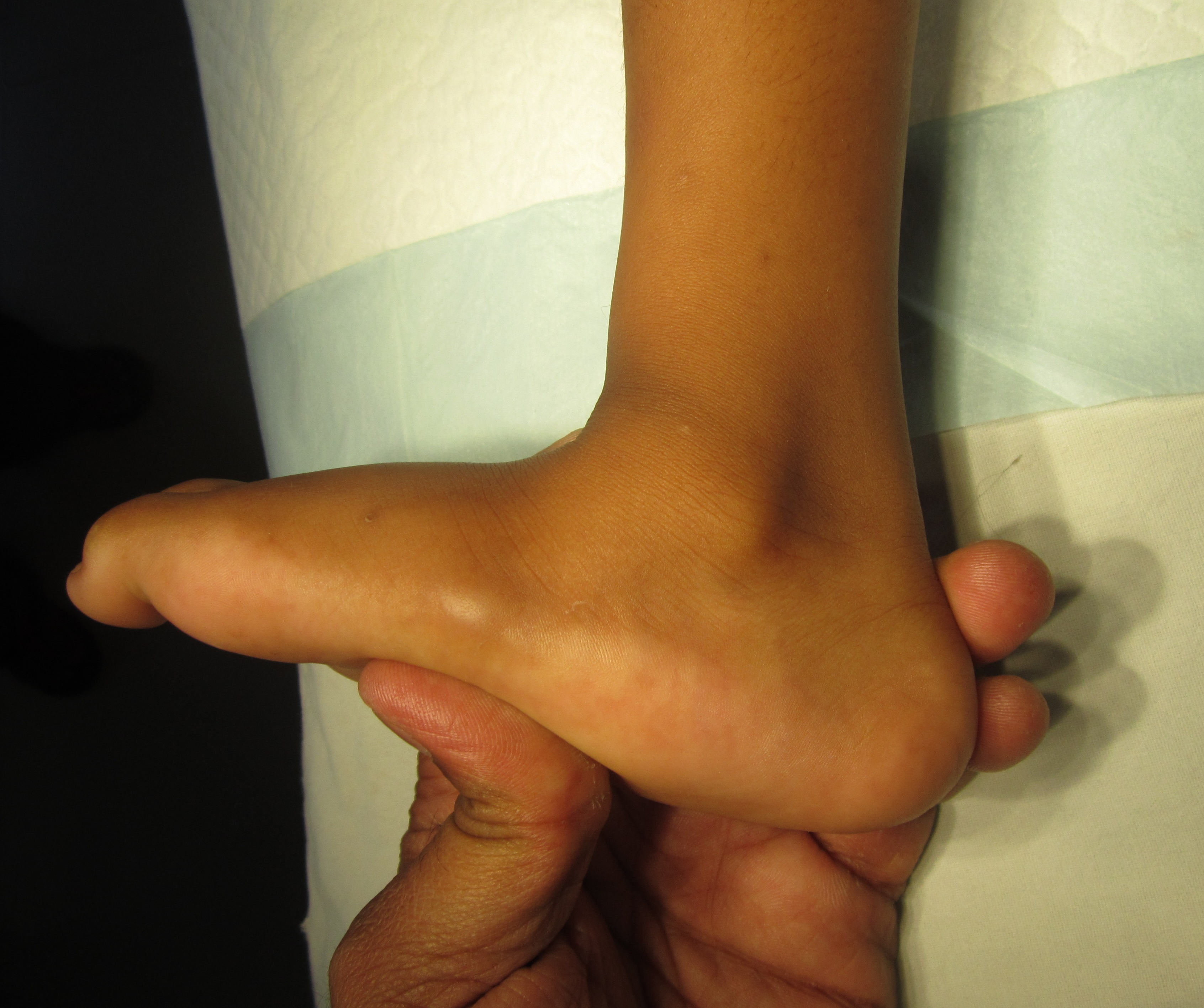
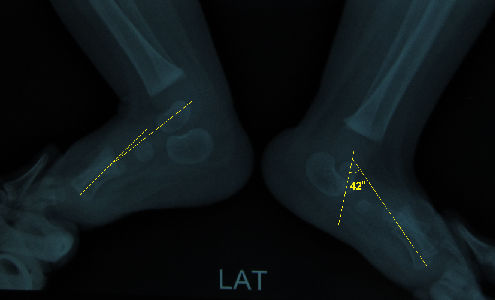
Illustration 2: Lateral view with forced plantar flexion showing vertical talus (talar- first metatarsal axis angle > 35?) on left foot.
Illusration 3: AP radiograph of foot showing Angle X – Talar first metatarsal axis angle and Angle Y – Talo calcaneal angle.
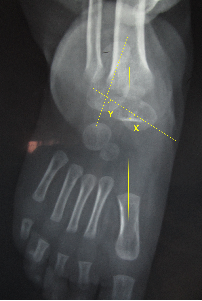
Illustration 4: Post op Xray showing Talo navicular joint reduced and fixed with a K wire.
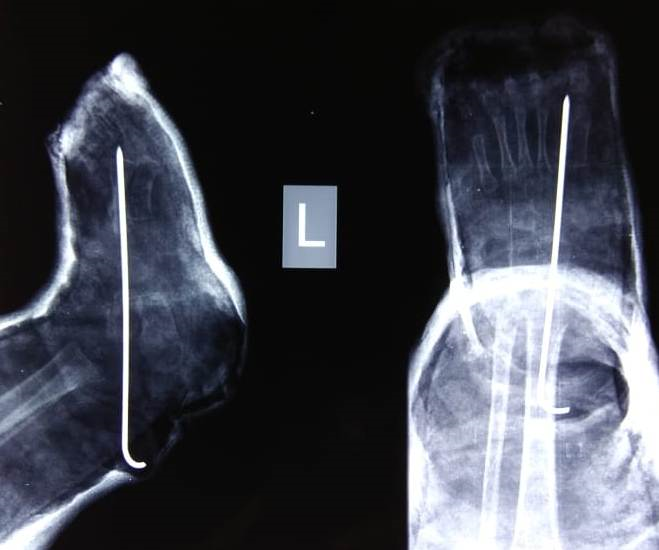
Source(s) of Funding
No source of funding
Competing Interests
No conflicting interests
 All site content, except where otherwise noted, is licensed under a
Creative Commons Attribution License
All site content, except where otherwise noted, is licensed under a
Creative Commons Attribution License